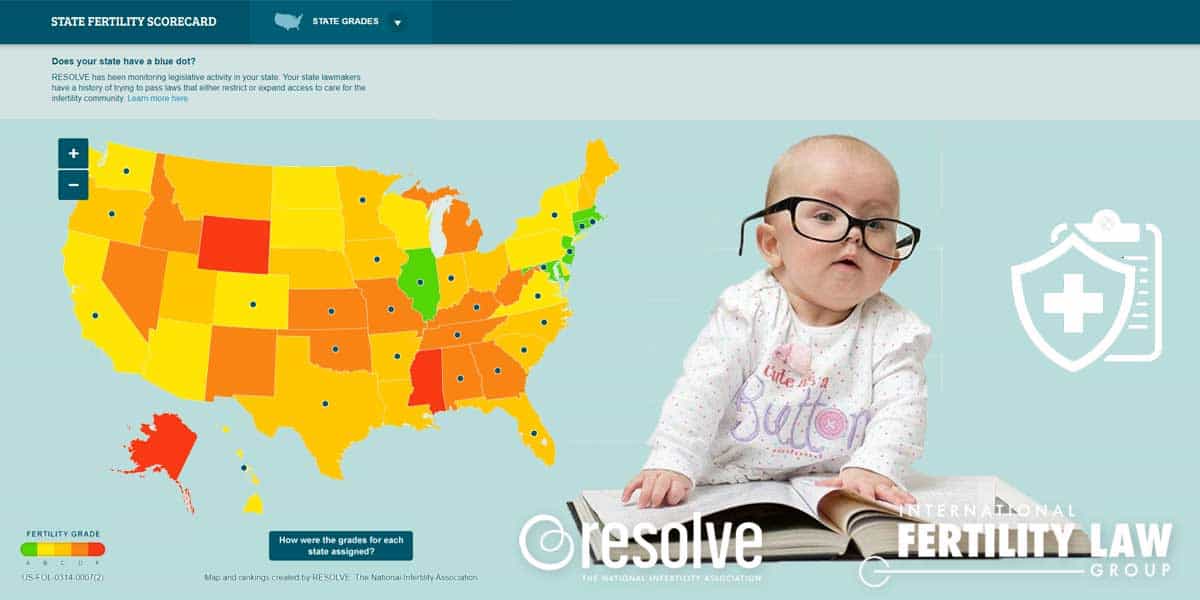
(image): Infertility Insurance Coverage By State and Scorecard Map from RESOLVE, a 501(c)3 nonprofit dedicated to ensuring that all people challenged in their family building journey reach resolution. Click HERE to learn more.
Even as a growing number of states require certain insurers to offer infertility insurance coverage, the details of who is required to provide coverage, who is eligible for coverage and what fertility treatments are covered vary widely from employer to employer and state to state.
As we have written, the U.S. Affordable Care Act left it up to each state to define the Essential Health Benefits (EHB) that insurers are required to cover. Consequently, ACA insurers may no longer cover some fertility treatments that were previously covered by state law.
For example, in April 2020, the state of New York passed a measure requiring insurance policies covering employee groups of 100 or larger to include coverage of in vitro fertilization, becoming the tenth state to require IVF coverage. The new law also includes expanded coverage for fertility-preservation efforts, such as egg or sperm freezing, for patients who require lifesaving but invasive medical treatments, such as radiation therapy, that may result in infertility.
California, in contrast, has for many years required insurers covering at least 20 employees to offer infertility treatment insurance, usually for a higher premium. In 2013 lawmakers passed legislation to clarify that the infertility insurance mandate covers LGBTQ intended parents.
In October 2019, the American Society for Reproductive Medicine (ASRM) reported on the results of Massachusetts’s infertility insurance mandate, considered the most longstanding and comprehensive in the country. Their conclusion? With exemptions for large, self-insured employers and public health insurance policies, only 36 percent of reproductive-age women in Massachusetts are covered by the mandate.
The National Conference of State Legislatures offers this state-by-state summary of infertility insurance coverage nationwide, citing the pertinent statutes.
Infertility Insurance Coverage Can Be Difference on Affordability
As we reported in 2014, for most intended parents considering assisted reproductive technology such as egg donation or sperm donation, in vitro fertilization (IVF) or surrogacy, the cost of ART
procedures is a serious consideration.
This dearth of infertility coverage leaves many infertile couples, to say nothing of single or same-sex intended parents, with a terrible choice. A single round of in vitro fertilization, in which an egg is fertilized with sperm outside of the womb, in a lab, can cost between $15,000 and $25,000; a single egg donation cycle is an additional $18,000 to $20,000.
Financially strapped intended parents whose health insurance does not cover IVF and egg donation costs too often feel pressure to maximize the odds of a successful pregnancy by having more than one embryo implanted—they simply cannot afford to come back for a second or third round.
Insurance coverage for even a portion of the cost of these highly specialized procedures can, for some intended parents, mean the difference between proceeding or not.
Intended parents should address questions about financing and insurance coverage directly with the donor or surrogacy agencies they are working with, as well as with their reproductive medical provider. An experienced fertility attorney also can provide referrals to insurance experts who specialize in ART and fertility insurance coverage.
Donor, Surrogacy Agreements Document Insurance Coverage
At IFLG, a New York surrogacy lawyer also will work with intended parents, surrogates and/or donors to draft surrogacy agreements customized to each individual situation. Generally, if a surrogate has medical insurance through her or a spouse’s employer, her insurance will cover basic healthcare and prenatal care during the course of the pregnancy. Typically, intended parents, or their insurer, are responsible for all costs of egg donor cycles and insemination procedures, as well as any medical costs resulting from pregnancy complications or delivery. The surrogacy agreement will establish each party’s responsibilities in each situation.
Since we launched IFLG to practice exclusively in fertility and the laws surrounding assisted reproductive technology, the trend has been toward expanding infertility insurance coverage, making ART more accessible for thousands of Americans. Just as laws governing parentage and assisted reproduction are a patchwork across the United States, so are laws mandating coverage for infertility treatment. For intended parents considering family-building with ART, a review of your health insurance coverage in consultation with the ART professionals with whom you are working is an important first step in realizing your dream.